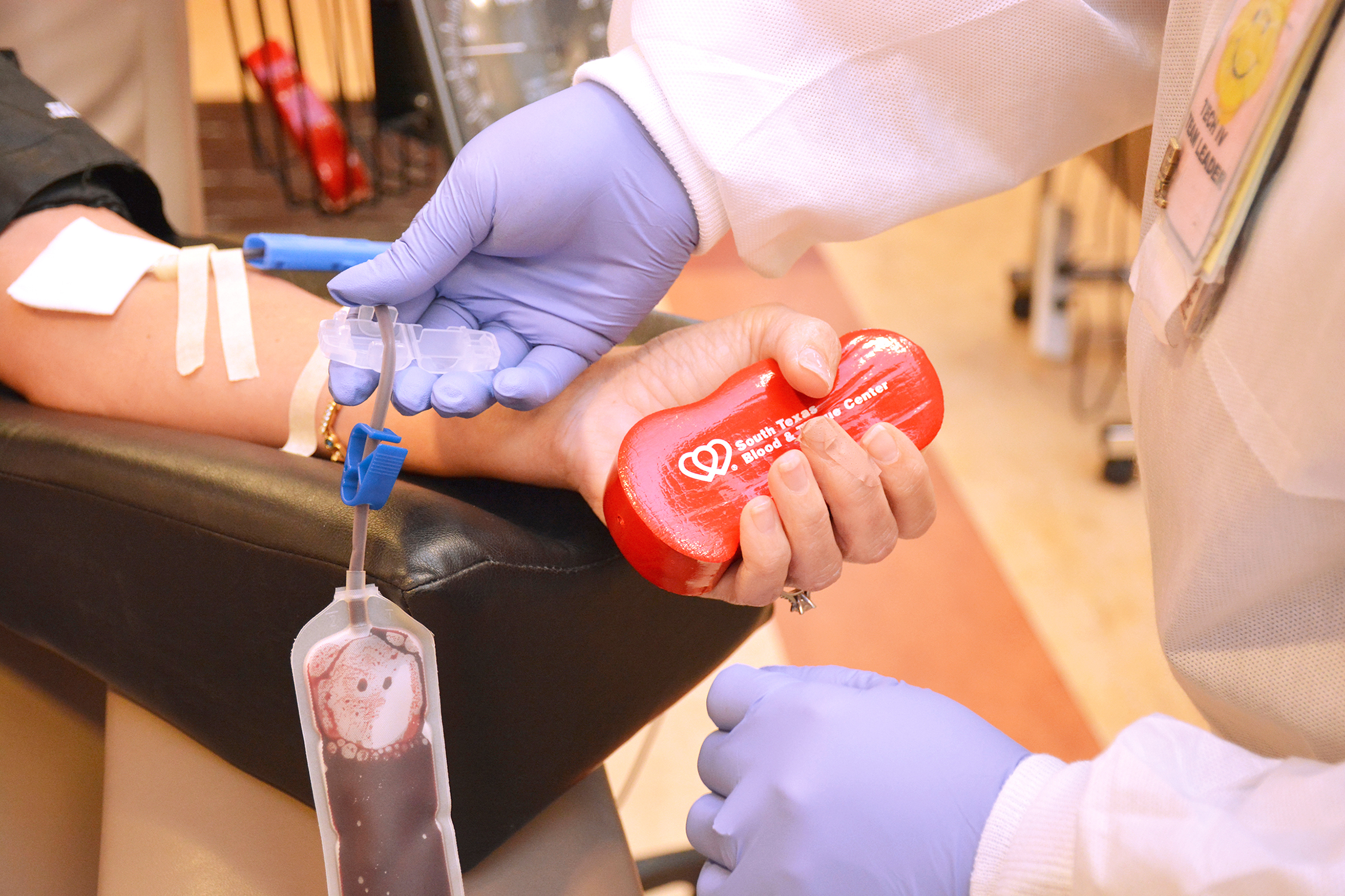
Every year, the most common reason donors can’t give blood is low iron levels.
The amount of iron in the body is determined by a number of factors, but younger women and frequent blood donors of either gender are particularly susceptible to levels below the threshold of safety as determined by the Food and Drug Administration.
Here are some commonly asked questions about iron and blood donations:
What happens to my iron during a blood donation?
Red blood cells are red because of the way iron is carried in hemoglobin, a protein that brings oxygen to the body. Therefore, the removal of red blood cells during blood donation also removes iron from your body.
The impact of this iron loss on your health varies among donors.
How does blood donation affect iron stored in my body?
Iron is needed to make new red blood cells to replace those you lose from donation. To make new red blood cells, your body either uses iron already stored in your body (referred to as your “iron stores”) or uses iron in the food you eat.
Many women have only a small amount of iron stores, often not enough to replace the red blood cells lost in a donation. Men have more iron stored in their bodies. However, men who donate blood often (more than two times per year) also may have low iron.
Does the blood center test for low iron stores in my body?
Not directly. The center tests your hemoglobin levels, since the iron is carried on hemoglobin. The test does not measure the body’s iron stores.
You may have a normal amount of hemoglobin and be allowed to donate, even if your body’s iron stores are low.
How may low iron affect me?
There are several possible symptoms associated with low iron, including fatigue, decreased exercise capacity, cognitive dysfunction, pregnancy complications and pica, which is the desire to compulsively ingest non-food substances such as ice or clay.
In addition, having low iron may increase the possibility of having a low hemoglobin test, preventing blood donation.
What can I do to maintain my iron?
Eating a well-balanced diet is important for all donors.
Choose iron-rich foods and add more Vitamin C to your diet such as green, leafy vegetables, beans, dried fruit and red meat or seafood. However, simply eating iron-rich foods may not replace all the iron lost from blood donation.
Either of the following supplementations would replace iron from a whole blood donation:
- A multivitamin with 18 mg iron taken for 60 days
- Elemental iron 18 mg taken daily for 60 days
Ask your physician or pharmacist for advice on what dose, type, and duration of iron supplement to choose. They also will be able to provide information on the effect of iron on absorption of other medications. See other tips to make your donation successful.
Why doesn’t a single big dose of iron replace what I lose during the donation?
Because people have a limit in iron absorption (around 2-4 mg/day), taking iron in larger doses for a shorter period may not lead to better absorption and may result in more side effects like digestive problems. The goal is to replace, in 30 to 90 days, the 200-250 mg of iron lost during donation.